Categories
Categories
- Home
- Natural Progesterone
- Oral vs Topical vs Vaginal vs Rectal vs Sublingual
Oral vs Topical vs Vaginal vs Rectal vs Sublingual
Topical, Oral, Sublingual, Vaginal, Rectal, Sublingual, and Injection Natural Progesterone
|
Contents |
|
|
4. Rectal And Vaginal Administration of Progesterone |
Topical Transdermal Progesterone
The following is a direct excerpt from John Lee, MD's book, "What Your Doctor May Not Tell You About Breast Cancer".
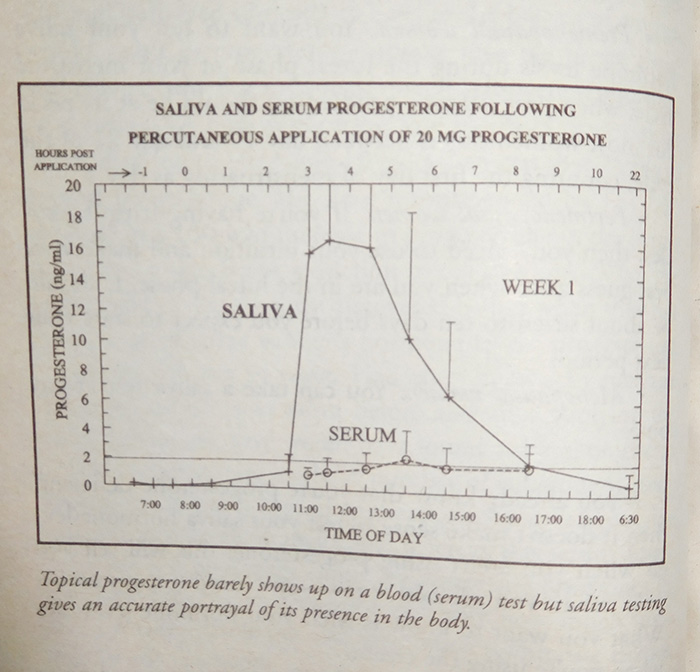
"When Progesterone is used transdermally, blood tests don't show a measurable rise, and this is why so many doctors believe it isn't absorbed. We'll explain why it doesn't show up in the chapter on progesterone, but for now what's important to take from this study is the fact that progesterone levels rose dramatically in the breast cells of women using transdermal progesterone, and this proves that progesterone is well absorbed when applied to the skin. The blood tests showed no measurable increase of progesterone concentration, however. This is an excellent illustration of the fact that blood testing can't be reliably used to determine the bioavailable level of progesterone when it's delivered through the skin, because very little bioavailable progesterone is carried in the blood plasma, which is what's measured in a standard blood test.
Dr. Zava has noted both in carefully controlled clinical studies and in daily testing of thousands of saliva samples that this same dosing of [topical transdermal] progesterone (about 20-30 mg) results in a remarkable increase in salivary progesterone, as much as 10 to 50 times, more closely reflecting what K.J. Chang and colleagues found in breast tissue uptake of these hormones. Two studies recently reported from Australia confirm that topical progesterone results in very little increase in serum progesterone but a remarkable increase in saliva levels of progesterone."[1]
Oral Progesterone Versus Topical Progesterone
John Lee, M.D. prefers to use topical progesterone. He points out that Mother Nature never puts progesterone in the stomach. The reason why is once the progesterone goes into the stomach liver first pass metabolizes progesterone by 90%. So, if you take a progesterone pill that is 200 mg, your body only gets 20 mg of that.
In contrast, if you put 20 mg of topical progesterone on the skin, the progesterone goes straight into the body and is not first pass metabolized by the liver. John Lee M.D. found that if the progesterone cream had mineral oil in it, the progesterone would be blocked by the mineral oil and the progesterone would not be absorbed.
I do not know exactly what the 90% metabolites of the progesterone does. However, I know that it makes my patients very sleepy. I had one patient that was taking 400 mg per day of progesterone orally to prevent miscarriage. She took the 400 mg of progesterone pills, and then traveled to Walmart by car. She was so sleepy at Walmart that she had to ask her husband to drive her back home. She was too sleepy to drive because of the metabolites created by taking 400 mg of progesterone by mouth. In contrast, 40 mg of topical progesterone, the same potency as 400 mg orally, will just make you a little sleepy. My patients usually like to take the progesterone just before they go to bed as it induces a very nice sleep.
Sublingual Administration of Progesterone
Some of my patients, have opted to use sublingual progesterone. This simply means to drop progesterone oil underneath the tongue, and hold it there. There is a large vein  underneath the tongue that absorbs the progesterone. I do not like to use this method unless the patient needs the progesterone immediately for a migraine headache. The reason why is that I don't know how long the patient will hold the progesterone oil underneath the tongue. So if the patient drops 100 mg underneath the tongue, and holds it there for an hour, maybe the patient will absorb most of the 100 mg through the vein. Maybe her body will get 100 mg of progesterone. However, if the patient holds the progesterone oil underneath the tongue for 5 minutes and then swallows it, maybe most of the progesterone will be absorbed orally and NOT by the sublingual vein, and 90% will be first pass metabolized by the liver. In this case, her body will get 10 mg of progesterone. So, if the patient takes 100 mg of progesterone sublingually, I am not sure whether her body is getting 10 mg or 100 mg. It depends how long she holds the progesterone oil underneath the tongue.
underneath the tongue that absorbs the progesterone. I do not like to use this method unless the patient needs the progesterone immediately for a migraine headache. The reason why is that I don't know how long the patient will hold the progesterone oil underneath the tongue. So if the patient drops 100 mg underneath the tongue, and holds it there for an hour, maybe the patient will absorb most of the 100 mg through the vein. Maybe her body will get 100 mg of progesterone. However, if the patient holds the progesterone oil underneath the tongue for 5 minutes and then swallows it, maybe most of the progesterone will be absorbed orally and NOT by the sublingual vein, and 90% will be first pass metabolized by the liver. In this case, her body will get 10 mg of progesterone. So, if the patient takes 100 mg of progesterone sublingually, I am not sure whether her body is getting 10 mg or 100 mg. It depends how long she holds the progesterone oil underneath the tongue.
However, some people need to take progesterone very quickly to stop their migraine headache, and they find that taking some sublingual progesterone is the perfect cure.
Rectal And Vaginal Administration of Progesterone
Some doctors say that progesterone can more easily be absorbed by the body by the vaginal or rectal mucosa. These doctors recommend the vaginal progesterone trouche or rectal trouche. In my opinion, if you want the effect of progesterone to be in the vaginal area more than normal, then I would recommend taking a progesterone trouche vaginally. Natural progesterone will increase vaginal lubrication. Some women have vaginal dryness, and progesterone in the vagina works great. Vaginal dryness is characterized by soreness and irritation, and is caused by xenoestrogens. Natural estriol can be used for vaginal atrophy. The skin on the vagina can become thin after menopause and the during intercourse this may result in tearing of the tissue with bleeding. Natural estriol can thicken up the skin of vagina and birth canal. Estriol and progesterone both go very high during the third trimester pregnancy. Sex drive goes through the roof. Estriol is used by the body during the third trimester to thicken up the skin. Estriol thickens and toughens the vaginal skin to prevent ripping as the baby travels through the birth canal.
So, if you have vaginal dryness, I recommend avoiding xenoestrogens and perhaps putting progesterone and natural estriol directly on the vaginal tissue.
However, that area of the body is drained by the rectal plexus. The rectal plexus is a network of veins that that drain in part to the portal vein. The portal vein goes straight to the liver. Therefore, some of the progesterone absorbed either by the rectum or vagina goes straight to the liver through the portal vein and is first pass metabolized 90%. Thus, progesterone absorbed by the vagina or rectum is less than the progesterone put onto the arm or leg or trunk. The total body dose taken up by the vagina or rectum is less than if you put natural progesterone on the skin directly.
I had one lady that had eight pregnancies, and on the ninth pregnancy she miscarried. She called me to try to prevent a miscarriage in her 10th pregnancy. I gave her 60 mg of topical progesterone per day for the first trimester. 30 mg in the morning. 30 mg at night. At week 16, I slowly tapered off progesterone. It is extremely important to slowly taper off the  progesterone. If you stop progesterone suddenly than the dropping progesterone levels will signal the body to have a miscarriage. So, I usually taper off progesterone over a period of six weeks. Her 10th pregnancy progressed with no difficulty. Baby came out fine.
progesterone. If you stop progesterone suddenly than the dropping progesterone levels will signal the body to have a miscarriage. So, I usually taper off progesterone over a period of six weeks. Her 10th pregnancy progressed with no difficulty. Baby came out fine.
On her 11th pregnancy, she did not consult me. She went to her doctor and asked for progesterone to prevent miscarriage. The doctor did not believe her, but on a whim prescribed 75 mg progesterone vaginal suppositories. She had a miscarriage. The reason why she had a miscarriage is that progesterone taken up by the vagina is drained in part by the portal vein. The portal vein goes straight to the liver. The liver 90% first pass metabolizes the natural progesterone. The reason why she had a miscarriage is that she did not get enough progesterone because she took progesterone by the vagina instead of putting it on topically on the skin.
Injection of Natural Progesterone
Subcutaneous injection of natural progesterone is also used and is very popular among infertility physicans. Natural progesterone is dissolved in a vegetable oil and injected on a periodic basis to keep and safeguard the baby. The shots typically are injected into the buttocks area. The one problem is that periodic injections are painful. In contrast, transdermal topical progesterone can safely be used to stop miscarriage. The only thing to remember is that topical trandermal natural progesterone must be taken twice a day because the natural progesterone levels go up and down in about 7 hours. The transdermal progesterone may be taken 3 times per day if necessary. It is also important to NOT forget to take the progesterone even one day. The dropping progesterone levels from forgetting to take the progesterone for one day will signal to the body to create a miscarriage.
1. Topical progesterone goes directly into the body whereas an oral progesterone pill is 90% first pass metabolized by liver. Thus, a 20 mg skin dose of progesterone is equivalent to a 200 mg progesterone pill taken orally.
2. Sublingual progesterone is good to stop migraines if you need any progesterone dose suddenly. However, the dose can be erratic because it depends on how long the patient keeps the progesterone under the tongue. If the patient puts the progesterone under the tongue, and then swallows and after short time, then, most of the progesterone would be taken orally. An oral dose must be divided by 10 compared to topical.
3. Rectal or vaginal suppositories of progesterone can be used especially if you want a local effect directly on the vagina. However, the body dose for a rectal or vaginal suppository would be lower than a topical skin dose because the rectum and vagina is in part drained by the portal vein. The portal vein goes straight to the liver. The liver then inactivates the progesterone by 90%. Thus, the rectal or vaginal suppository gives a lower total body dose of progesterone. However, as some physicians point out the rectal or vaginal mucosa may provide better absorption. On a woman that is heavy set, this may be true. Personally, if the patient is heavy set, I tell the patient to apply the progesterone on the inside of the arms and thighs where the subcutaneous fat is thin. If the patient is NOT heavy set, then she may apply the topical progesterone anywhere on the body where the circulation is good. She may apply the progesterone to the arms, legs, chest, back, neck, or face. She may rotate areas every day. If she keeps doing right arm every day, the subcutaneous fat will saturate and her body canNOT absorb any more progesterone. This is why it is important to rotate areas.
Notes:
1. John Lee, MD, David Zava, PhD, and Virginia Hopkins, What Your Doctor May Not Tell You About Breast Cancer, Hachett Book Group USA, 2005, pages 127-128.
 Loading... Please wait...
Loading... Please wait...