Categories
Categories
Miscarriage
Miscarriage and Natural Progesterone
Miscarriage during 5 to 8 weeks of gestation is usually due to a natural progesterone deficiency. This is known as a corpus luteum defect. The corpus luteum simply does not produce enough progesterone. All you have to do is to take a progesterone blood level and compare it with a normal progesterone blood level for the week of gestation. If the progesterone blood levels are low, then this would explain the miscarriage. Mainstream physicians routinely give progesterone supplementation for women having a miscarriage between 5 to 8 weeks for progesterone deficiency. They usually measure blood levels of natural progesterone, and if they are found below compared to normal, they will give progesterone supplementation.
See My Beautiful Baby Boy!
I felt compelled to email you and thank you. It has been over a year since I contacted you for progestelle for my low progesterone in early pregnancy. Since then, my beautiful, healthy baby boy was born in February. He is such a blessing to us and our older kids. I can't thank you enough for your help and availability and this product. I am so happy to hold my baby and watch him grow. Thank you, thank you, thank you!
With warm regards,
Blessings,
Amy V. Minnesota, June 29, 2017
It was certainly a testimony to my midwife too, she was wonderful and supportive. Even though the blood tests stayed low, just like you said they would. I also made a number of changes based on reading your information as well. Even though I try to eat healthy, I realized it wasn't enough, body products and soaps matter too!

Actual picture of patient's new baby boy. This is not a model.
Sometimes different herbs can cause miscarriage. Aloe and mint are two examples of herbs in folk medicine used to create miscarriage. In certain cultures, if you do not want your pregnancy if you drink enough aloe juice during the first trimester it will cause a miscarriage. I do not agree  with this morally. However, many times there will be aloe in shampoos, lotions, cosmetics, and lipsticks. Just as nicotine patches are made to deliver nicotine transdermally to the body, these lotions, shampoos and cosmetics will transdermally deliver aloe to the body. Could transdermally delivered aloe cause a miscarriage? I don't know. But I think it would be unwise to use toiletries that contain aloe during the first trimester of your pregnancy.
with this morally. However, many times there will be aloe in shampoos, lotions, cosmetics, and lipsticks. Just as nicotine patches are made to deliver nicotine transdermally to the body, these lotions, shampoos and cosmetics will transdermally deliver aloe to the body. Could transdermally delivered aloe cause a miscarriage? I don't know. But I think it would be unwise to use toiletries that contain aloe during the first trimester of your pregnancy.
I also believe that it would be unwise to use any herb considered in the folk medicine to traditionally cause a miscarriage during your pregnancy. During the 1930s, some of these herbs that facilitated abortion were used in the medications to stop cramping. These herbal medications were banned by the US government because they were dangerous to potential pregnancies.
I want to go on record as saying that I am not against herbs. If I am a male and I went to the beach and got a sunburn, I would certainly use aloe on my sunburned skin to alleviate the burn. Aloe is a great herb for burns. Aloe can strengthen the immune system. However, aloe is traditionally used to create miscarriages in the first trimester. Thus, if you are female and are potentially pregnant, the use of aloe would be unwise and contraindicated. You really have to know what are doing. You must respect herbs, you can't just use herbs willy-nilly. Many of our modern medications are from herbal folk medicine. For instance, the digoxin used to increase contractility of the heart for congestive heart failure was originally from an Irish tea from the foxglove plant.
The Use of Natural Progesterone for Miscarriage
In my book, a miscarriage from 5 to 8 weeks is a progesterone deficiency until proven otherwise, or an herb that causes miscarriage. I usually give 30 mg of progesterone transdermally in the morning, and 30 mg of progesterone transdermally in the evening. The levels of progesterone go up and down in about seven hours according to the hormone levels that John Lee, MD took in the book, "What Your Doctor May Not Tell You About Breast Cancer". You can take progesterone supplementation for the first trimester, and then slowly taper it off over a period of several weeks. The reason  why progesterone has to be tapered off slowly over a period of several weeks is that if you stop the progesterone suddenly, this signals the body to create a miscarriage. So, it is important to take the progesterone every single day. If you forget to take the progesterone just one day, the dropping of progesterone levels will signal to the uterus to create a miscarriage. Therefore, you must not run out of progesterone. Do not skip one day of progesterone, otherwise, the dropping progesterone levels will create a miscarriage. Always have extra progesterone in reserve. Do not stop taking progesterone for any reason at all during the first trimester.
why progesterone has to be tapered off slowly over a period of several weeks is that if you stop the progesterone suddenly, this signals the body to create a miscarriage. So, it is important to take the progesterone every single day. If you forget to take the progesterone just one day, the dropping of progesterone levels will signal to the uterus to create a miscarriage. Therefore, you must not run out of progesterone. Do not skip one day of progesterone, otherwise, the dropping progesterone levels will create a miscarriage. Always have extra progesterone in reserve. Do not stop taking progesterone for any reason at all during the first trimester.
If you're still having cramps in contractions during 5 to 8 weeks at 60 mg of progesterone a day, you can easily go up on progesterone and double it to 120 mg per day transdermally. You may even use 200 mg a day transdermally of natural progesterone. You may increase the natural progesterone suddenly. The only thing that you may NOT do is to decrease the progesterone suddenly. Again, any time you decrease the progesterone suddenly this signals to the body that a miscarriage should occur. If you suddenly stop the progesterone, this will cause a miscarriage. Remember during one day of third trimester pregnancy, your body produces 400 mg of progesterone per day. So let's assume that if you put 200 mg transdermally on your skin, there is a 50% absorption rate. That is only 100 mg, and then that is one quarter of one day of third trimester pregnancy.
Natural progesterone is produced by the corpus luteum in the first trimester of the pregnancy at about 20 to 60 mg per day. Progesterone production continues to ramp up throughout the entire pregnancy. During the second and third trimesters of pregnancy, the placenta forms and matures and makes the majority of progesterone for the woman during that time. The contribution to progesterone by the corpus luteum during the second and third trimesters is relatively minor compared to the placenta's contribution.The placenta begins to make massive amounts of progesterone to the tune of 400 mg per day during one day of third trimester. Thus, usually, a miscarriage from 5 to 8 weeks results from not enough production of progesterone by the corpus luteum. Thus, usually, if there is a corpus luteum defect, progesterone only needs to be given during the first trimester. However, there is some cases, about 10% of them where I began to taper off the progesterone at 16 weeks and the woman began to have contractions. Why was that?
Use of Natural Progesterone Throughout the Entire Pregnancy
These 10% women start to have contractions when I began to taper off progesterone at 16 weeks usually were very allergic or had Hashimoto's thyroiditis. They were allergic to many different things. They may have had a hypersensitivity to smell before they got pregnant. They had a positive Romberg test. (A Romberg test is where you put your feet together and stand on your tip toes, and close your eyes. Women that were positive for the Romberg test would wobble.) They may get seasick when they go in a boat on the ocean. They were sensitive to small amounts of drugs. If you gave them a 500 mg dose of caffeine, and measured their blood levels of caffeine 24 hours later, you would find it elevated. These women are collectively known as chemically sensitive. If they walked down the detergent aisle in the grocery store they would find the perfumes offensive and sometimes have a headache from the perfumes. All these allergies are usually due to fear, stress, anxiety, elevating histamine and interleukin six levels. At any rate, these women would seem to have antibodies to everything. It is my hypothesis that these women may have had antibodies to progesterone itself.
The progesterone produced by your body is bound by a binding protein, which makes it water-soluble. Progesterone normally is not water soluble. Progesterone normally dissolves in oil. Progesterone is oil soluble. So the body makes a binding protein that binds to the progesterone that makes the progesterone water-soluble. Is my hypothesis that antibodies in the water-soluble fraction of your blood can then attack to the progesterone that is bound to the binding proteins that are water-soluble.
 Transdermal natural progesterone is in contrast, not bound to the binding protein. Transdermal natural progesterone is found in the chylomicrons (little droplets of oil in the blood), and on the red blood cell membranes. Antibodies found in the water fraction of the blood cannot attack the transdermal progesterone found in the chylomicrons and red blood cell membranes because oil and water don't mix. Therefore, these patients that are extremely allergic and begin to have contractions when you taper off Natural progesterone transdermally respond quite well to transdermal natural progesterone taken throughout the entire pregnancy.
Transdermal natural progesterone is in contrast, not bound to the binding protein. Transdermal natural progesterone is found in the chylomicrons (little droplets of oil in the blood), and on the red blood cell membranes. Antibodies found in the water fraction of the blood cannot attack the transdermal progesterone found in the chylomicrons and red blood cell membranes because oil and water don't mix. Therefore, these patients that are extremely allergic and begin to have contractions when you taper off Natural progesterone transdermally respond quite well to transdermal natural progesterone taken throughout the entire pregnancy.
There is no danger to taking progesterone throughout the entire pregnancy. It will just cost you more money. The only danger is if you forget to take the natural progesterone transdermally for one day, the dropping progesterone levels will cause a miscarriage. Taking natural progesterone thoughout the entire pregnancy will not make your gestation time any longer. A normal gestation time is 40 weeks. Taking progesterone right up to delivery on the 40th week will not prolong your pregnancy. Other hormones will kick in to help deliver your child. A month of progesterone used to maintain your pregnancy is about $50. This is a small price to pay for a healthy child. Again, taking 60 mg per day transdermally is a small percentage of what your body is making during one day of third trimester pregnancy (400 mg/day). The 60 mg per day transdermally will not prevent delivery. Other hormones like oxytocin and prostaglandins will kick in and allow labor and delivery to occur. Again, the supplemental progesterone will not stop the baby from the baby from being delivered at the correct time.
If the child is delivered prematurely before full-term, the child will go into the neonatal intensive care unit. The cost treating a child in the neonatal intensive care unit is anywhere between $50,000-$100,000. However, that's not the major problem. The major problem is that the child will have permanent disabilities ranging from cerebral hemorrhages and lung problems. Because the surfactant needed to fully inflate the lungs has not developed for these preterm delivery babies, usually there is scar tissue in the lungs. $50 of transdermal progesterone per month is really cheap.
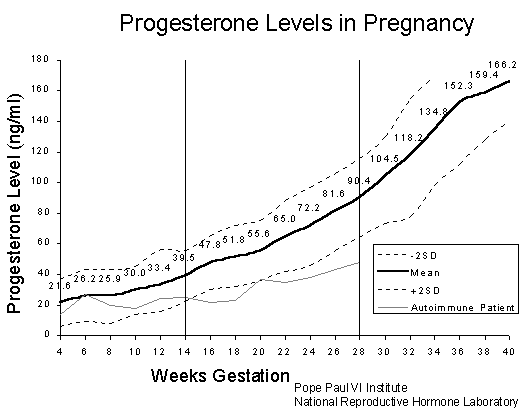
Note the grey line in the chart above. The grey line is the concentration of progesterone for women with autoimmune disease. It may be extremely important for women with autoimmune disease to take progesterone for the entire pregnancy because women with autoimmune disease have low progesterone. So, if you are a woman with autoimmune disease, make sure to take progesterone throughout the entire pregnancy.
Time Magazine Showcases the Use of Natural Progesterone to Prevent Miscarriage
Time Magazine published an article on January 10, 2017 on the use of Progesterone Cream, Vaginal Progesterone, or Oral Progesterone to prevent miscarriage. You can read the article here if the link is still live. Stephenson, MD of the University of Illinois, demonstrated that vaginal micronized progesterone 100-200 mg/every 12 hours stopped early miscarriage. Women were treated from 2004 to 2012 with unexplained pregnancy losses earlier than 10 weeks. Women that had endometritis, maturation delay, glandular-stromal dyssynchrony as identified on endometrial biopsy were excluded from the study. Vaginal micronized progesterone 100-200 mg every 12 hours was given to women having increased glandular nuclear E (nCyclinE) or empirically (having normal nCyclinE). nCyclinE is a blood test marker predicting miscarriage. The higher nCyclinE, the more the risk for miscarriage. Women that had recurrent miscarriage given progesterone had increased pregnancy success.
116 women were enrolled in the study. 59 women had elevated nCyclinE. 57 women had normal nCyclinE. Pregnancy success in 59 women with elevated nCyclinE had significant success with their pregnancy. 6% success in prior pregnancies compared to 69% success in the progesterone prescribed pregnancies. Even women with normal nCyciinE, had higher success in pregnancy taking progesterone as compared to not taking progesterone 68% vs 51%.
Stephenson, MD notes in the Time Magazine article that Progesterone Cream, Vaginal Progesterone, and Oral Progesterone can all be used to prevent miscarriage. She published her results in the Journal of Fertility and Sterility. [0]
University of Birmingham Suggests the use of Progesterone to Prevent Some Miscarriages
Research done by the University of Birmingham suggests new guidelines to help thousands of women with prior miscarriage and bleeding in early pregnancy keep their pregnancy. Updated guidance, was announced on November 24, 2021 by the National Institute for Health and Care Excellence (NICE). The evidence was revealed by two trials named PRISM and PROMISE by the University of Birmingham and Tommy's Centre for Miscarriage Research.
NICE recommends giving progesterone to women who have early pregnancy bleeding and have had a previous miscarriage. An ultrasound scan should be done to confirm a healthy pregnancy and then the pregnant patient should be given progesterone until week 16. NICE found that there was no benefit in giving progesterone to women with early pregnancy bleeding but no previous miscarriage. NICE also found that women with previous miscarriage but no bleeding in early pregnancy also had no benefit from progesterone.
PROMISE studied 836 women with unexplained recurrent miscarriages at 45 hospitals in the UK and the Netherlands, and found a 3% higher live birth rate with progesterone, but with substantial statistical uncertainty.
PRISM studied 4,153 women with early pregnancy bleeding at 48 hospitals in the UK and found there was a 5% increase in the number of babies born to those who were given progesterone who had previously had one or more miscarriages compared to those given a placebo. The benefit was even greater for the women who had previous ‘recurrent miscarriages’ (i.e., three or more miscarriages) – with a 15% increase in the live birth rate in the progesterone group compared to the placebo group.[17]
Of the newly updated NICE guidance, Arri Coomarasamy, Professor of Gynaecology & Reproductive Medicine at the University of Birmingham and Director of Tommy’s National Centre for Miscarriage Research who led the PRISM and PROMISE trials, said: “After many years researching the use of progesterone and working to make treatment more accessible, today’s new miscarriage care guidelines from NICE include a very welcome change. Our research has shown that progesterone is an effective and safe treatment option, which could prevent 8,450 miscarriages a year in the UK – but we know it’s not yet reaching everyone who might benefit. This recommendation from NICE is an important step in tackling the current variation in miscarriage services across the country and preventing these losses wherever possible.”
Topical Transdermal Natural Progesterone Versus Oral Natural Progesterone Versus Rectal or Vaginal Natural Progesterone
The normal dose to prevent miscarriage in the first trimester is 60 mg/day of transdermal natural progesterone per day divided into two doses of 30 mg in the morning and 30 mg in the evening. Is important to remember that anything orally is 10 times less in potency than what is taken on the skin. Therefore, an oral dose of progesterone needed to stop miscarriage is 400 to 600 mg per day taken orally. Rectally or vaginally progesterone trouches are used. Rectally or vaginally the blood is drained by the rectal plexus. The rectal plexus is in part drained by the portal vein. The portal vein goes straight to the liver and first pass 90% inactivates progesterone. Thus, the progesterone trouche needs to be much more than 60 mg per day, otherwise a miscarriage may occur.
I had one patient that had eight children. Then, she had two miscarriages, during the 5 to 8 weeks of gestation period. So, she called me and I recommend 60 mg progesterone per day given transdermally for the first trimester. Her ninth child carried to term uneventfully. There was no problem in the pregnancy. Then, she became pregnant again. She did not talk to me. She visited her doctor and insisted she needed additional progesterone to maintain the pregnancy. The doctor was skeptical, but prescribed her a 75 mg vaginal progesterone trouche suppository. She had a miscarriage. The reason why is 75 mg per day of progesterone taken vaginally is less than 60 mg of progesterone taken transdermally on the skin. Again, progesterone taken vaginally or rectally is in part drained by the portal vein which goes straight to the liver and is 90% first pass inactivated.
Topical Transdermal Natural Progesterone Cannot be Observed in the Blood Test - Use a Saliva Test
It is important to realize that topical natural progesterone that is transdermally absorbed will not appear in the progesterone blood test. You cannot measure transdermal natural progesterone absorption by using the blood test. Do not use the blood test to measure transdermal natural  progesterone absorption. You can only use the saliva test to assess transdermal natural progesterone absorption. Many physicians assume that because the blood test does not show progesterone levels that the transdermal progesterone is not being absorbed by the body. This is a wrong assumption. Please do not use blood tests to assess transdermal progesterone use. Again, transdermal progesterone is in the body in the chylomicrons, the little oil droplets in the blood, and the red blood cell membranes. The blood test measures progesterone in the water fraction of the blood. However, transdermal progesterone is not in the water fraction of the blood. Transdermal natural progesterone is in the oil fraction of the blood which the blood test does not measure. Thus, you cannot assess progesterone levels in the body from a progesterone cream by using the blood test. You must use a saliva test to measure transdermal natural progesterone absorption.
progesterone absorption. You can only use the saliva test to assess transdermal natural progesterone absorption. Many physicians assume that because the blood test does not show progesterone levels that the transdermal progesterone is not being absorbed by the body. This is a wrong assumption. Please do not use blood tests to assess transdermal progesterone use. Again, transdermal progesterone is in the body in the chylomicrons, the little oil droplets in the blood, and the red blood cell membranes. The blood test measures progesterone in the water fraction of the blood. However, transdermal progesterone is not in the water fraction of the blood. Transdermal natural progesterone is in the oil fraction of the blood which the blood test does not measure. Thus, you cannot assess progesterone levels in the body from a progesterone cream by using the blood test. You must use a saliva test to measure transdermal natural progesterone absorption.
Less than 1% of patients do not absorb topical progesterone well. According to Wright, MD of the Tahoma Clinic, these patients were obese and heavy set. They used progesterone over the fatty layers of their body. Thus, the progesterone was absorbed into the fat and was not "seen" by the body. He told these obese patients to use the progesterone on the insides of the arms and insides of the thighs where the subcutaneous fat was thinner. Then, these patients that "did not absorb progesterone well" were able to absorb progesterone well. Also, in these patients, oral natural progesterone may be used. However, you must use oral progesterone at levels of 400 mg to 600 mg per day. Anything taken orally is 90% first pass inactivated by liver. So, oral progesterone taken at 400 mg to 600 mg per day is equivalent to the body getting 40 mg to 60 mg a day. Transdermal natural progesterone is 10 times in potency than whatever you take orally. Thus, a 60 mg transdermal natural progesterone does is equivalent to a 600 mg per day oral dose. Whatever is taken transdermally bypasses the liver and goes straight into the body. Example of this action is nicotine patches found at the drugstore. Nicotine is in the drug patch is put a put on the skin and is absorbed directly into the body. You may also use progesterone injections. You may also use vaginal or rectal progesterone suppositories at levels well above 60 mg per day. This is because the vaginal and rectal regions of the body is in part drained by the portal vein which goes straight to the liver. The liver will first pass 90% inactivate any progesterone that comes to it through the portal vein.
Do Not Take Progesterone Before You Ovulate-If You Are Trying to Get Pregnant
Do not take progesterone before you ovulate, if you're trying to get pregnant. The ovaries will look for the progesterone levels in the body and if they see progesterone levels in the body, they will think that you are already pregnant. Then, they will not ovulate. So, taking progesterone before ovulation will stop ovulation. Therefore, if you want to get pregnant, do not take progesterone before you ovulate. Instead, you may take progesterone after you ovulate. Taking progesterone, after you ovulate, will actually increase your fertility because it stimulates the uterine lining to differentiate into a nice nest for the embryo can implant. Therefore, I usually recommend taking 60 mg per day of progesterone after you ovulate. Then, at day 28, you can use "First Response" pregnancy test. "First response" pregnancy test can be found in any large department store and is one of the most reliable pregnancy tests. Do not use other pregnancy tests. If you are pregnant at day 28, then continue to use progesterone at 60 mg a day. If you are not pregnant at day 28, then you can stop the progesterone. Again, if you are pregnant at day 28 continue to use progesterone at 60 mg day. Stopping the progesterone suddenly will cause a miscarriage. After week 16 of gestation, you may taper off the progesterone very slowly over period of four weeks. You may email us if you have bought a product from us, for the exact protocol.
Take Folic Acid to Prevent Spina Bifida - Methylated Folic Acid is Better
It is important to take at least 1000 µg of folic acid to prevent spinal bifuda. Some doctors actually recommend more than that. Some sources even even hint that at least 50% of the population have methylation defects, and some patients cannot use folic acid because they cannot methylate it. These people believe that you should be taking a methylated folic acid. These methylation problems can also be linked to having problems maintaining the pregnancy. Dr. Ben Lynch N.D. may be a good resource for the methylation defect or MTHFR defect. You can take a genetic test at "23 and me" to see if you have methylation problems or simply take methylated B vitamins.
Take Chromium to Prevent Gestational Diabetes
Gestational diabetes is caused by a chromium deficiency. There are no chromium deposits in North and South America. Well, there is some chromium in Brazil. There is chromium in Africa, Asia and Europe, but little or no chromium in North and South America. No chromium deposits in North and  South America in the soil means that the grass has no chromium in it. The beef that eats the grass has no chromium in it. After you eat the beef, you don't get any chromium. Therefore, almost the entire population of North America is chromium deficient. Chromium is a cofactor to be used with insulin. Chromium nicotinate can be used to reverse gestational diabetes. Jovanic reported that 8 mcg/kg per day given to gestational diabetic women significantly lowered post meal glucose levels. [1] For a 120 pound woman, this would be a dose of 400 mcg of chromium nicotinate per day. Baker et al. stated that high doses of chromium 1000 mcg/day resulted in improved glucose tolerance in a population of diabetes type II in China. [2] www.medscape.org/viewarticle/490853_5
South America in the soil means that the grass has no chromium in it. The beef that eats the grass has no chromium in it. After you eat the beef, you don't get any chromium. Therefore, almost the entire population of North America is chromium deficient. Chromium is a cofactor to be used with insulin. Chromium nicotinate can be used to reverse gestational diabetes. Jovanic reported that 8 mcg/kg per day given to gestational diabetic women significantly lowered post meal glucose levels. [1] For a 120 pound woman, this would be a dose of 400 mcg of chromium nicotinate per day. Baker et al. stated that high doses of chromium 1000 mcg/day resulted in improved glucose tolerance in a population of diabetes type II in China. [2] www.medscape.org/viewarticle/490853_5
Andrew Weil, MD believes that you should take 1000 mcg/day of GTF chromium. GTF chromium is actually chromium with niacin and glutathione. A recent study from University of California showed chromium polynicotinate was absorbed and retained 311% better than chromium picolinate.[3] There was one small study on young overweight women at the University of Texas. They gave 400 mcg/day to obese women of chromium picolinate and chromium nicotinate with and without exercise. Chromium picolinate resulted in weight gain. Chromium nicotinate resulted in significant weight loss especially when combined with exercise.[4]. Another study showed that chromium picolinate may cause DNA damage in the test tube.[5-7] However, the DNA damage could not be replicated in the human body.[8]
Take Chromium Nicotinate, Chromium Polynicotinate, or GTF Chromium - NOT Chromium Picolinate
Many studies demonstrate the safety of taking 1000 mcg/day of chromium for several months.[9-10] However, there were three individual cases involving chromium picolinate that had a bad outocome. One case reported kidney failure five months after a six week course of 600 mcg/day of chromium picolinate.[11] One 33 year old woman had kidney failure and impaired liver function was reported in one use of 1200 to 2400 mcg/day of chromium picolinate over a 4-5 month time. She returned to normal after supportive measures were taken.[12] Another 24 year old male took a supplement containing chromium picolinate developed reversible acute renal failure after taking the supplement for 2 weeks. [13] If you have liver disease or a kidney condition extra care should be taken to take chromium picolinate.
I could not find any adverse cases taking chromium involving chromium nicotinate, chromium polynicotinate, or GTF chromium. At any rate, I recommend 400 mcg/day or more (some recommend levels as high as 1000 mcg/day) of chromium nicotinate, chromium polynicotinate, or GTF chromium. I am not recommending chromium picolinate at this time because of these few adverse reactions by 3 individuals.
Take a Good Prenatal Vitamin 90 Days Before Conception
Both you and your spouse should take a good prenatal vitamin 90 days before conception. All veterinarians know this. Both the egg and the sperm are in suspended animation. Both the egg and the sperm are "asleep". Then, 90 days before conception, both egg and sperm wake-up, and begin to take in nutrition to build up themselves for conception. Thus, ninety days before conception, it is very important to provide proper nutrition for both egg and sperm. Animal husbandry managers know this. Preconception nutrition is extremely important. Also, any drugs prescription, or over-the-counter, or natural herbs with therapeutic effects should be carefully scrutinized in the ninety days before conception and during the pregnancy. I had one patient that had trouble conceiving because the husband was on over-the-counter cold medications which affected the sperm morphology. Once the husband stopped taking the over-the-counter cold medications, the couple conceived.
Iodine Supplementation BEFORE Pregnancy
50% of Europe is mildly iodine deficient. [14] Brownstein, MD tested 500 patients in the Midwest United States and found 95% of them to be iodine deficient. The gold standard is to five a 50 mg oral dose of iodine, then to collect a 24 hour urine. If you get 80% of the iodine back, then you are iodine sufficient. If you get less than 80% back, then your body is still keeping iodine.
A 2013 review article by Karim Bougman about iodine supplementation research studies about iodine supplementation and depletion relating to the IQ of children under 5 years old summarized articles on Medline and PubMed from January 1980 to November 2011. He also searched the references identified in the those studies as well. He found 24 relevant studies. There were four types of studies:
1. Radomized control studies, individuals or communities received iodine supplements compared to placebo.
2. Non Randomized control studies, individuals or communities received iodine supplements compared to placebo.
3. Prospective cohort, women were grouped according to iodine nutrition (deficient or not) and followed up to delivery.
4. Prospective cohort, infants with varying iodine nutrition from congenital hypothyroidism were given iodine supplementation and then were followed for several years.
Many of the control studies both randomized and not randomized used single doses of 950 mg and 450 mg because those studies were done in developing countries such as Ecuador or China. The area had severe areas of goiter ranging from 54% to 83% The studies done in Spain were 300 mcg of iodine per day. These supplementation levels in Spain were much too low according to the data from Abraham, MD of optimox corp. makers of Iodoral. The studies done in the prospective cohort studies were from “iodine sufficient” regions such as the United States, Canada, Italy, and the Netherlands. However, in Flechas, MDs, Abraham, MD, and Brownstein, MD opinion, the women in the United States are 95% of the time insufficient in iodine. The studies generally agreed that early supplementation prior to conception or early in pregnancy showed consistent benefits. Iodine supplementation late in pregnancy did not have benefits. Intervention studies on the mental outcome of children 5 years old showed an increase of 7.4 IQ points. Iodine supplementation before or during early pregnancy had more benefit than late pregnancy supplementation.
First trimester normal levels of iodine mothers were correlated with children with consistently increased mental development in nine different studies. The difference in iodine sufficient mothers versus iodine deficient mothers was 7.8 IQ points. [15]
In one small study involving 40 school children aged 7-13, the children were divided into 3 groups. The first group, the mothers received iodine oil 1-4 years before conception and the infants received iodized salt from 1-4 years. The second group, the mothers had iodized oil during pregnancy and the infants received iodized salt from 2-4 years. The third group of children received iodized oil injections from years 1-3 and iodized salt from ages 3-6. They compared their IQ results with a control group that were age and sex matched. Mean IQ for group one was 102. Mean IQ for group two was 93. Mean IQ for group three was 95. They concluded that children of mothers receiving iodine supplementation before conception had significantly higher IQ values then women receiving iodine during pregnancy or after birth.[16]
I think it is important to take iodine before you conceive. Make sure that any bromine detox is over before your pregnancy takes place.
Magnesium Deficiency Leads to Uterine Cramping and Possible Miscarriage
Women that have Estrogen Dominance from chronic xenoestrogen exposure typically have a magnesium deficiency. The sure sign that you have a magnesium deficiency is that you have a chocolate craving just before your period. Chocolate is one of the foods with highest concentration of magnesium. If you have a magnesium deficiency, then you will crave magnesium. In the medical world, this is known as a pica. Craving magnesium leads to craving chocolate.
If you have a chocolate craving, this means a magnesium deficiency. A magnesium deficiency means that your muscles will tense up and contract. The uterus is simply an upside down muscular “sack”. Because of the magnesium deficiency, the uterus will cramp up and this may lead to a miscarriage. It is extremely important to take an easily absorbable magnesium. I prefer Magnesium Citrate at 200-800 mg/day. If you start to get loose stools or diarrhea, then cut back on the magnesium. Do NOT take magnesium oxide as magnesium oxide may only have an absorption rate of 4%.
Summary for the Use of Natural Progesterone in Pregnancy.
1. Usually a miscarriage occurring from 5 to 8 weeks is a progesterone deficiency, or you are being exposed to an herb that causes miscarriage.
2. If you begin to taper off the progesterone at week 16 and begin to have contractions, go back up on the progesterone and use it throughout the entire pregnancy. If you have an autoimmune disease, your progesterone during the pregnancy will be low. If you have an autoimmune disease, take progesterone throughout the entire pregnancy.
3. Do not forget to use progesterone for one day. If you forget to use progesterone for just one day, the dropping progesterone levels will cause a miscarriage. Again, do not run out of progesterone. You must take progesterone every day, otherwise a sudden stopping of progesterone will cause a miscarriage.
4. Topical transdermal natural progesterone can only be assessed by the saliva test. A blood test will not show transdermal natural progesterone.
5. Take at least 1000 µg per day of folic acid per day to prevent spina bifida.
6. Take 400 µg per day of chromium nicotinate, chromium poly nicotinate, or GTF chromium to prevent and perhaps even reverse gestational diabetes.
7. You and your spouse should be taking a good prenatal vitamin 90 days before conception. No drugs even over-the-counter drugs should be taken at this time.
8. Take iodine at 12.5 mg/day 90 days before conception. Taking iodine before may increase your child's IQ by 7-10 IQ points. Watch out for bromine toxicity. Buy any product from us and get the protocol for taking iodine.
9. If you have a chocolate craving before your period, this signals that you are deficient in magesium. Magnesium deficiency is linked to uterine cramping and miscarriage. Take magnesium in order to stop cramping and possible miscarriage.
Notes:
0. Mary D. Stephenson, M.D., M.Sc., Dana McQueen, M.D., M.A.S., Michelle Winter, M.D., Harvey J. Kliman, M.D., Ph.D. Luteal start vaginal micronized progesterone improves pregnancy success in women with recurrent pregnancy loss, Fertility and Sterility, Jan. 9, 2017.
1. Jovanovic L., DruzinM, Peterson CM. Effect of euglycemia on the outcome of pregnancy in insulin-dependent diabetic women as compared with normal control subjects. Am J Med. 1981;71:921-927.
2. Baker JP, Haber GB, Gray RR Handy S. Emphysematous cholecystitis complicating endoscopic retrograde cholangiography. Gastrointest Endosc. 1982;28:184-186.
3. Gabriel Cousens, There is a Cure for Diabetes: The Tree of Life 21-Day+ Program
4. Grant KE, Chandler RM, Castle AL, Ivy JL, Chromium and Exercise Training: effect on obese women, Med Sci Sports Exerc. 1997 Aug;29(8):992-8.
5. Blasiak J, Kowalik J., A comparison of the in vitro genotoxicity of tri- and hexavalent chromium. Mutat Res. 2000; 469(1):135-145.
6. Speetjens JK, Collins RA, Vincent JB, Woski SA. The nutrtional supplement chromium(III) tris(picolinate) cleaves DNA. Chem Res Toxicol. 1999;12(6):483-487.
7. Stearns DM, Wise JP, Sr., Patierno SR, Wetterhahn KE. Chromium(III) picolinate produces chromosome damage in Chinese Hamster ovary cells. FASEB J. 1995;9(15):1643-1648.
8. Kato I, Vogleman JH, Dilman V, et al. Effect of supplementation with chromium picolinate on antibody titer to 5-hydroxymethyl uracil. Eur J Epidemiol. 1998;14(6):621-626.
9. Anderson RA, Cheng N, Bryden NA, et al. Elevated intakes of supplemental chromium improve glucose and insulin variables in individuals with type 2 diabetes. Diabetes. 1997;46(11):1786-1791.
10. Hathcock JN. Vitamins and minerals: efficacy and safety. Am J Clin Nutr. 1997;66(2):427-437.
11. Wasser WG, Feldman NS, D'Agati VD. Chronic renal failure after ingestion of over-the-counter chromium picolinate. Ann Intern Med. 1997;126(5):41.
12. Cerulli J, Grabe DW, Gauthier I, Malone M, McGoldrick MD. Chromium picolinate toxicity. Ann Pharmacother. 1998;32(4):428-431.
13. Wani S, Weskamp C, Marple J, Spry L. Acute tubular necrosis associated with chromium picolinate-containing dietary supplement. Ann Pharmacother. 2006;40(3):563-566.
14. Endocr Rev. 2009 Jun;30(4):376-408
15. Karim Bougma, Frances E. Aboud, Kimberly B. Harding and Grace S. Marquis, “Iodine and Mental Development of Children 5 Years Old and Under: A Systematic Review and Meta-Analysis”, Nutrients 2013, 5, 1384-1416; doi:10.3390/nu5041384
16. Salarkia N, Mirmiran P, Azizi F. “Timing of the Effect of Iodine Supplementation on Intelligence Quotients of Schoolchildren,”Int J Endocrinol Metab 2004; 2:95-102
17. https://www.birmingham.ac.uk/news/latest/2021/11/miscarriage-guidance-progesterone-research-arri.aspx
 Loading... Please wait...
Loading... Please wait...